Mental Health & Wellbeing Checklist
You are viewing a factsheet on Tune in Not Out, a health and wellbeing portal, view more topics here. We hope this factsheet below helps you…
It’s healthy to check in on ourselves now and then. It can help us identify areas which may need attention to improve our health and wellbeing.
The simple checklists will help you check in with how you’re faring. Yow can download a copy of this brochure here or view it as a flipbook.
Checklist 1: General Wellbeing
Before you begin…
This factsheet will ask you a series of questions about your health and wellbeing. Based on your answers, you will be given some feedback and advice.
Answer as honestly as you can for the most accurate results. The results are a guide and meant to be used as part of your decision making process. You are the expert on your body and life: take whatever action you feel is right for you.
These tests have been adapted from the open-source Psycheck screening tool for mental health symptoms, and the criteria from the Diagnostic and Statistical Manual of Mental Disorders 5th Edition (DSM-5) for substance use disorders.
The checklists & their results
The checklists can give you feedback, but they cannot provide a diagnosis. The results are a guide rather than a set of instructions. If the results don’t feel right to you, that’s okay. Take any action that meets your needs.
If any questions in the checklist raise concerns about your wellbeing, you can always reach out for help and guidance. The end of the factsheet has a list of services that can provide support.
Think of the checklists as a guide rather than instructions.
If you are worried, help is available.
Checklist 1: General Wellbeing
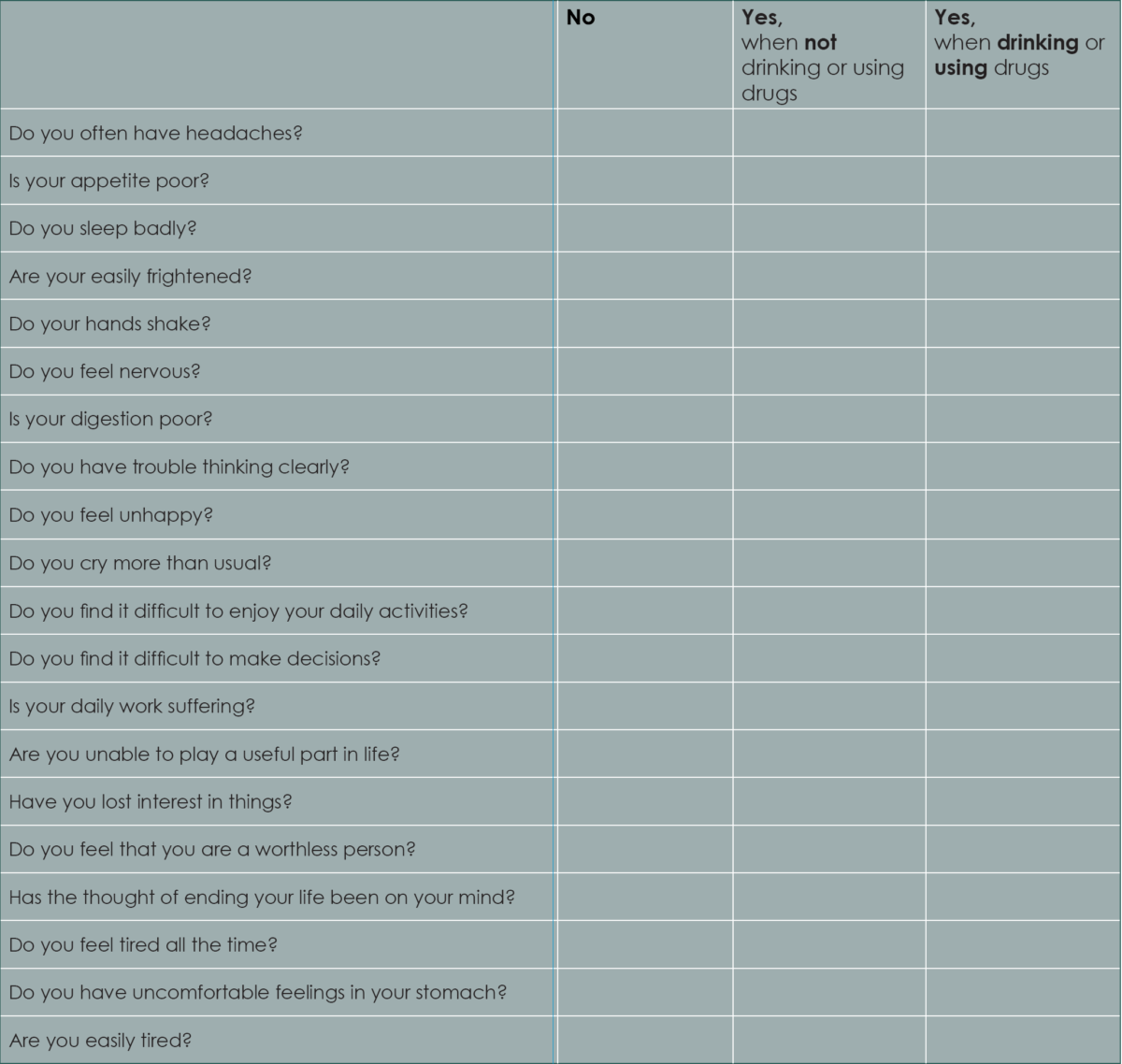
Checklist 1: The Results
If you said ‘no’ to every symptom this suggests you’re doing well. If you’re worried about anything, speak to your GP or someone you trust: it’s always OK to reach out for help.
If you answered “Yes, when not drinking or using drugs” for 1 to 4 questions this suggests you have some difficult symptoms. Speak to your GP or someone you trust – there is help available if you need or want it.
If you answered “Yes, when not drinking or using drugs” for 5 or more questions: You seem to have some difficult symptoms and having a hard time. Speak to your GP about your symptoms, or look at the end of this factsheet for some more specific help. It’s always OK to reach out for help, and you are not alone.
If you answered “Yes, when drinking or using drugs” for 5 or more questions, you might be having some problems related to alcohol or drug use. Take a look at the next checklist to see how you’re doing.
If you ticked yes to ‘when using alcohol and other drugs’, now complete the 2nd checklist below to see how you are doing….
Checklist 2: Alcohol & Other Drugs
Once you have completed the General Wellbeing Checklist above, it may have prompted you to complete this checklist.
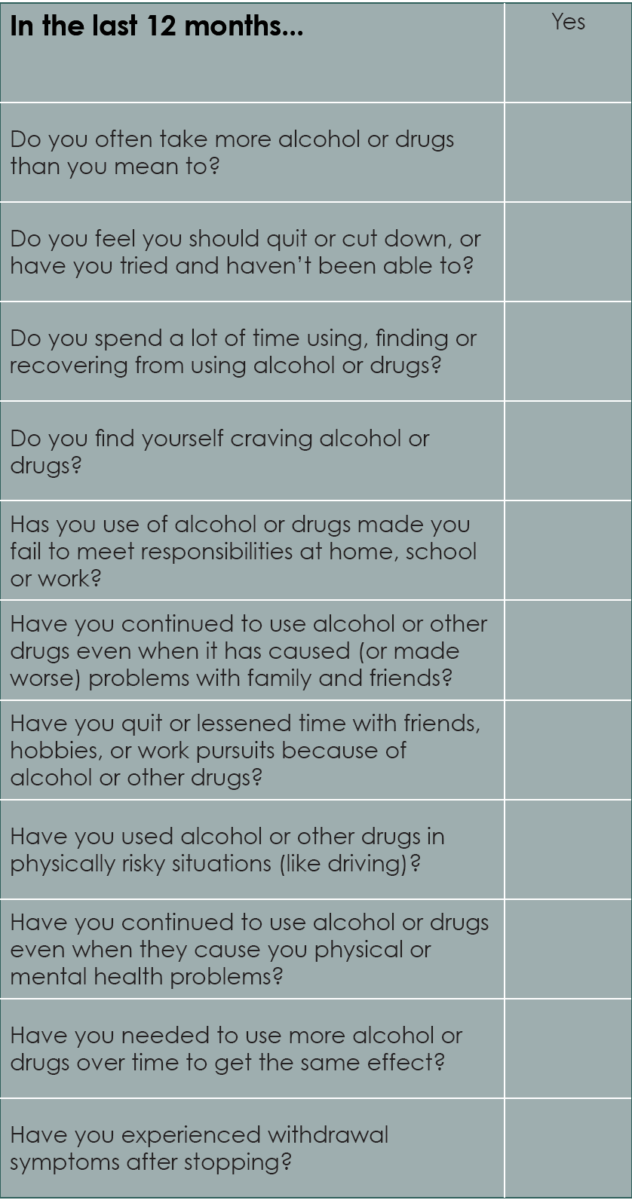
Checklist 2: The Results
If you answered Yes to 0-1 questions: This suggests you’re doing OK. Keep an eye on any symptoms, and don’t hesitate to reach out for help if you need it.
If you answered Yes to 2-3 questions: You might be having some mild problems with alcohol/ drugs. Consider speaking to your GP, and keep an eye on your symptoms.
If you answered Yes to 4 or more questions: You may be having moderate to severe problems with alcohol/drugs. Speak to your GP, or reach out to a specific alcohol and drug service. There are many services available to help you deal with any problems and work with you to achieve your goals for improving your wellbeing. Find out more about seeking help.
Whatever your results you are not alone.
There are many services that can help you, from websites with tips for staying well, to your local GP or support services to help you ensure you have a healthy relationship with alcohol other and other drugs.
Help and Info
If you’d like to speak to someone, local treatment services will be able to provide support for you and your family, and can answer any questions you may have about your wellbeing and health changes.
- Parents, Elders and trusted friends
- GPs and Pharmacists
- Local Alcohol and Other Drug Services – look under A in the phone book
- Other helping services like Youth, Mental Health or Disability services
- Lifeline Australia 13 11 14
- Kid’s Helpline 1800 55 1800
- Poisons Information Centre 13 11 26
- National sexual assault, domestic and family violence helpline 1800 RESPECT
- Family Drug Support a 24/7 service fds.org.au or 1300 368 186
- www.everybodys.business
- Medicines Line 1300 MEDICINE
- Get the effects by txt! 0439 TELL ME Simply text the name of the drug you want to know about
You can find other information our topic pages – view them all here.
Also check the related topics:
Depression Stress Suicide Psychosis and other mental illnesses Self harm Eating Disorders Anxiety Alcohol Inhalents Cannabis Ecstasy, ICE and other Amphetamines





